When community health worker Jerome Gardiner was growing up, there was no health clinic nearby. There wasn’t even a midwife, he recalls. For his community and rural communities throughout Liberia, this meant that potentially treatable conditions could become deadly, due to lack of access to basic health services.
Now, Jerome is one of 4,000 Liberian community health workers providing care for their neighbors in communities beyond the reach of the health system. Through Liberia’s National Community Health Assistant Program, those in rural and remote communities can access essential health services right at their doorsteps. “It doesn’t matter where you eat or where you live, opportunity can come,” reflects Jerome.
In Grand Bassa County, Liberia, where Jerome lives and works, Last Mile Health has supported the Ministry of Health to manage the implementation of the national program since 2018. The program was rolled out there in four phases, creating a unique opportunity to analyze its impact.
A recent paper published by Last Mile Health in PLOS Global Public Health reports results from the first phase of implementation. The paper’s authors compared areas with and without the program to answer three questions:
- First, were there larger increases in child healthcare in intervention areas than in areas where implementation had not yet begun?
- Second, if gains were observed, did the source of care shift to community health workers and facility-based providers from less effective informal sector providers?
- Third, how did changes in child healthcare in implementation areas vary across three measures of inequity: relative poverty, geographic remoteness, and maternal education?
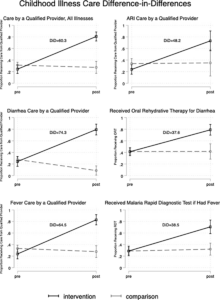
Results from Last Mile Health’s study on the implementation of the National Community Health Assistant Program in Grand Bassa County, Liberia.
Findings
Child healthcare: Between the pre- and post-intervention periods, care for childhood illness by a qualified provider increased by 60.3 percentage points more in intervention areas than comparison areas. The evaluation further identified large improvements in two important components of care: receipt of oral rehydration therapy for diarrhea and rapid diagnostic testing for malaria.
Care by a qualified provider: Care by a community health worker in intervention areas increased from 0% to 81.6% and care from unqualified providers decreased.
Equity in care delivery: Increases in care by a qualified provider did not vary significantly by household wealth, remoteness, or maternal education. This means families in more remote locations and those with fewer financial resources or lower educational attainment benefited equally in increased access to care, which is a core goal of the program.
This study found evidence that Liberia’s National Community Health Assistant Program led to substantial improvements in care coverage for childhood fever, diarrhea, and acute respiratory infection. This means more healthy–and happy–children and families.
Reflecting on his work in Grand Bassa County, Jerome Gardiner shares, “People have a saying, they say, ‘A healthy child, a happy mother.’ When I help the community and everyone is happy, I feel good.”
As Liberia works to sustain the National Community Health Assistant Program across 14 counties, continued monitoring and evaluations like this one are essential to ensuring the provision of high-quality care.





